Daily screen exposure has reached unprecedented levels across work, education, and entertainment. Alongside this shift, Computer Vision Syndrome has become an increasingly discussed concern in occupational and general health contexts. While often framed as a localized eye discomfort issue, growing attention suggests it may contribute to broader systemic symptoms, including headaches, neck tension, and reduced concentration.
Rising Digital Visual Demand
In modern environments, visual tasks are no longer intermittent but continuous, with prolonged near-focus work becoming a defining feature of daily life. Extended use of computers, smartphones, and tablets places sustained demand on the visual system, particularly in maintaining focus, eye alignment, and depth perception. Over time, this persistent workload may contribute to discomfort that extends beyond the eyes themselves. Individuals may report difficulty sustaining attention, visual blur during screen use, or a sense of ocular fatigue that accumulates throughout the day. These experiences are increasingly recognized in occupational health discussions as part of a broader pattern associated with digital lifestyles, rather than isolated eye strain events.
Computer Vision Syndrome as Systemic Strain
Computer Vision Syndrome is commonly described as a collection of visual and ocular symptoms associated with prolonged digital device use. However, emerging perspectives suggest its impact may not be confined to the eyes alone. Sustained visual effort can interact with posture and musculoskeletal tension, potentially contributing to symptoms such as tension headaches, shoulder stiffness, and neck discomfort. These manifestations are often interpreted as generalized stress responses, yet they may reflect a more integrated visual-physical strain pattern. The relationship between visual load and bodily discomfort highlights the interconnected nature of the visual system with broader neuromuscular function. As a result, Computer Vision Syndrome is increasingly considered in discussions that extend beyond ophthalmic health into overall well-being in digitally intensive environments.
Misattribution in Primary Care Settings
In many cases, individuals experiencing persistent headaches or neck pain initially seek evaluation through a family doctor. Because symptoms such as fatigue, tension, and reduced concentration are common across multiple conditions, they may be attributed to stress, lifestyle factors, or musculoskeletal strain. While these considerations are clinically relevant, they can sometimes obscure the potential contribution of visual system dysfunction. As a result, underlying visual strain may remain unaddressed when symptoms persist despite general interventions. This overlap in symptom presentation can make it challenging to distinguish between primary stress-related conditions and those influenced by visual effort, particularly in individuals with high daily screen exposure. Improved awareness of this overlap may support more comprehensive assessment pathways.
The Role of Optometric Evaluation
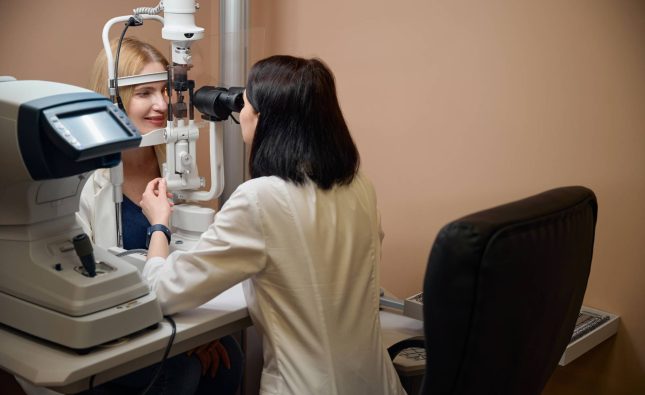
A specialized optometric evaluation may include assessment of binocular vision dysfunction, focusing on how the eyes coordinate during near tasks. In some individuals, subtle misalignment or focusing inefficiencies can increase the effort required for sustained visual work. This added effort may contribute to fatigue and secondary symptoms that extend beyond the visual system. An optometrist can assess these functional aspects of vision that are not always detected in routine screening. In this context, the role of optometry becomes part of a broader diagnostic picture, helping to differentiate between primary ocular conditions and functional visual stress. Such evaluation can provide additional clarity for both patients and their family doctor when exploring persistent symptom patterns.
Integrating Visual Insights Into Primary Care Understanding
When visual evaluation insights are shared with primary care, it may support more integrated understanding of multisystem symptoms. Framing persistent discomfort through both visual and systemic perspectives can help refine clinical hypotheses and reduce ambiguity in symptom interpretation. This collaborative lens does not replace existing diagnostic processes but adds an additional dimension to them. In this way, visual health assessments may contribute to a “clearer view” of chronic symptom patterns, ensuring that the visual system is considered as part of the broader physiological network influencing daily function in a digital environment. This perspective is not intended to replace medical evaluation but to complement it in understanding complex symptom clusters in modern work environments. It encourages interdisciplinary communication between vision specialists and primary care providers navigating digital-era health concerns.
In the context of rising screen dependency, Computer Vision Syndrome is increasingly discussed as more than an isolated eye concern. Its potential links to headaches, neck tension, and reduced concentration highlight the importance of considering visual health within broader wellness evaluations. While interpretations may vary, the integration of optometric assessment into symptom analysis can offer additional perspective for patients and healthcare providers. Ultimately, understanding the visual system as part of overall physiological balance may support more comprehensive approaches to persistent digital-age discomfort.